Healthcare
Elevate the patient experience with a virtual health agent who is on call 24/7.
Healthcare Resources Stretched Thin
Healthcare providers face the ongoing challenge of reducing costs while striving to meet the rising expectations of patients. Missed appointments alone cost the US healthcare system a staggering $150B1 every year. With mounting pressures to utilize resources more effectively, healthcare organizations are turning to conversational AI technology to handle the complexity around scheduling and automate common healthcare-related tasks.
1 Source: https://clinmedjournals.org/articles/jfmdp/journal-of-family-medicine-and-disease-prevention-jfmdp-4-090.pdf
AI Self-Service for the Patient Journey
SmartAction eases the burden on inundated contact centers while improving patient access to services. With our integration to major EHR systems, patients can book, reschedule, get wait-listed, and cancel appointments without waiting for human assistance. Our intelligent virtual health agents engage patients conversationally to handle inbound and outbound billing inquiries, help triage symptoms, and much more for a truly frictionless experience.
ROI from Scheduling Alone*
For many healthcare organizations, the conversational AI journey starts by automating scheduling over voice and digital channels. Here’s the ROI hospitals experience from this use case alone:
call reduction to
the contact center
average cost
savings per call
improvement in Net
Promoter Score
*Results averaged across SmartAction customers.
Proven Use Cases for Healthcare
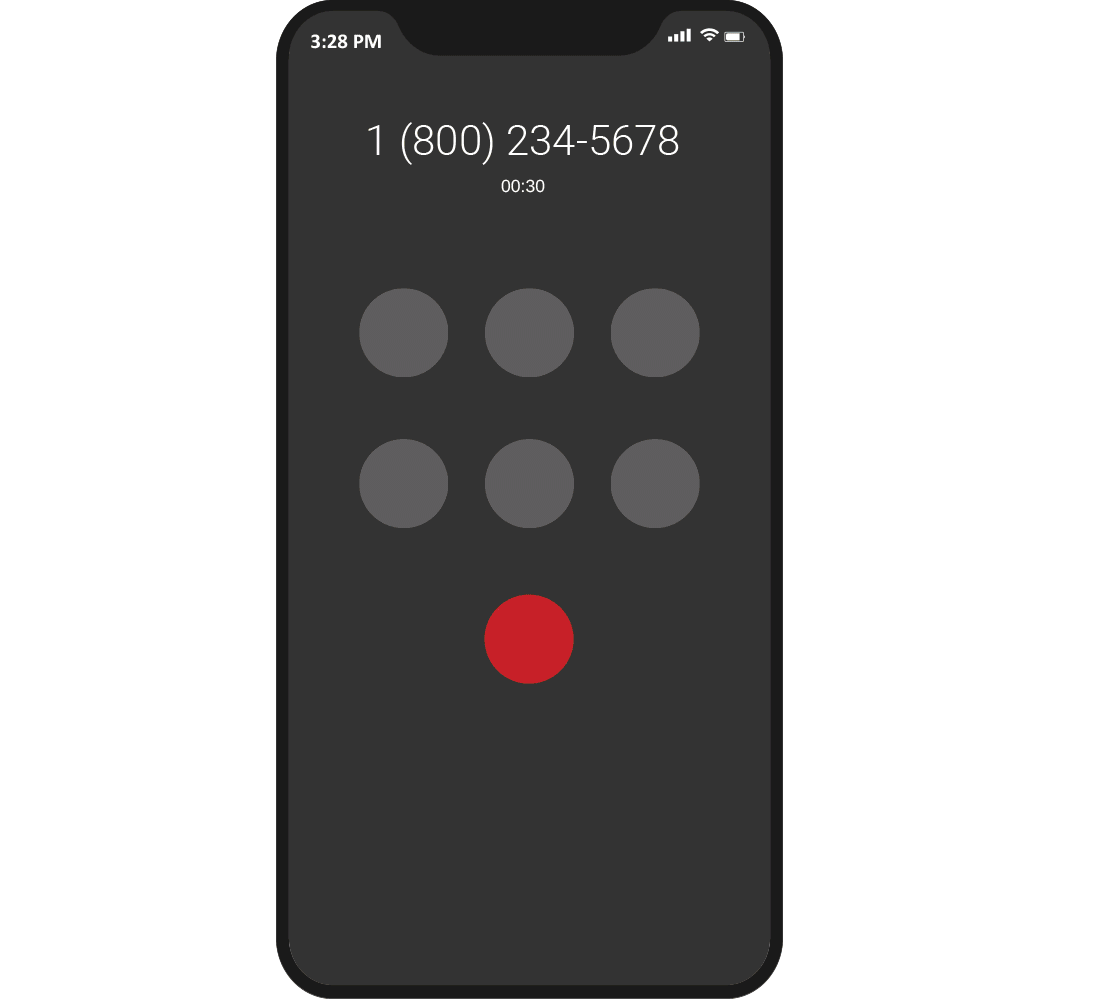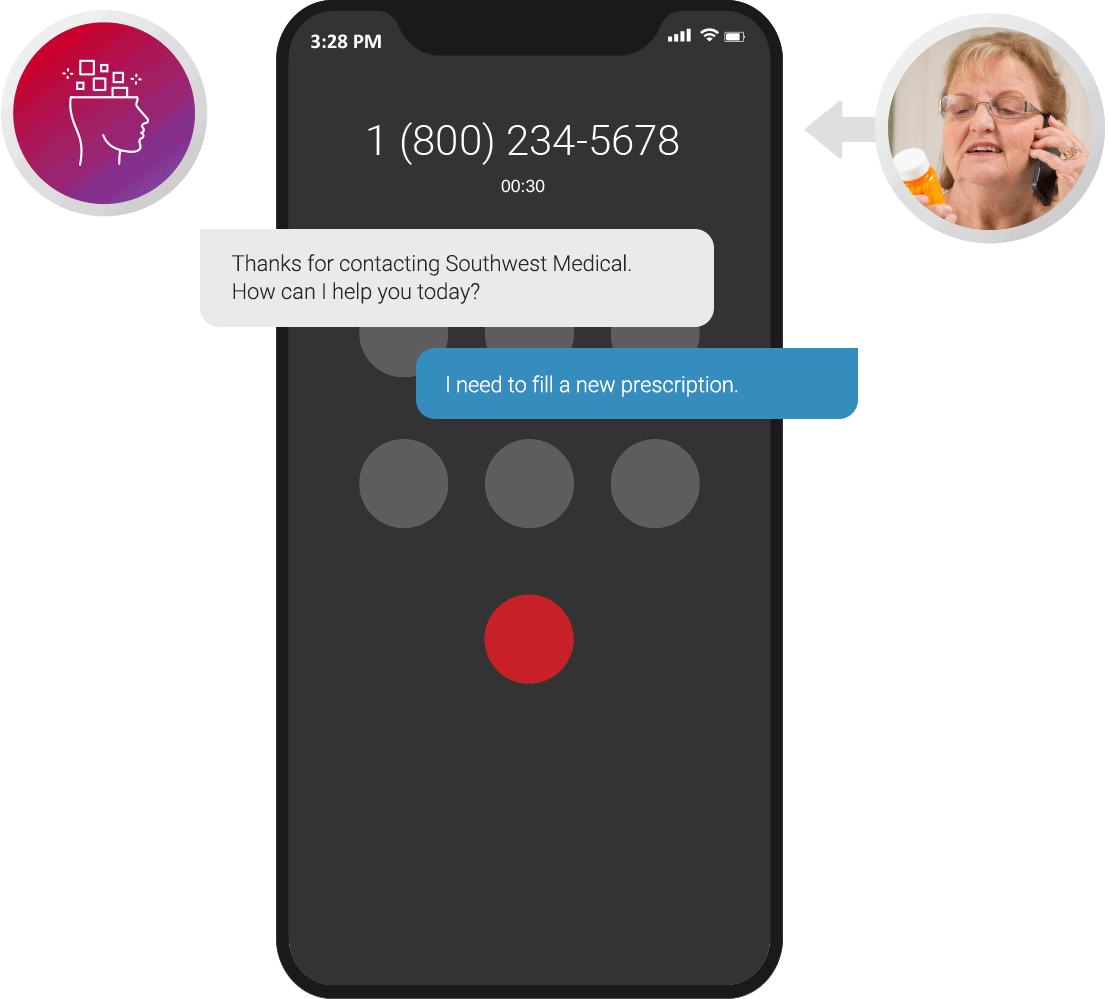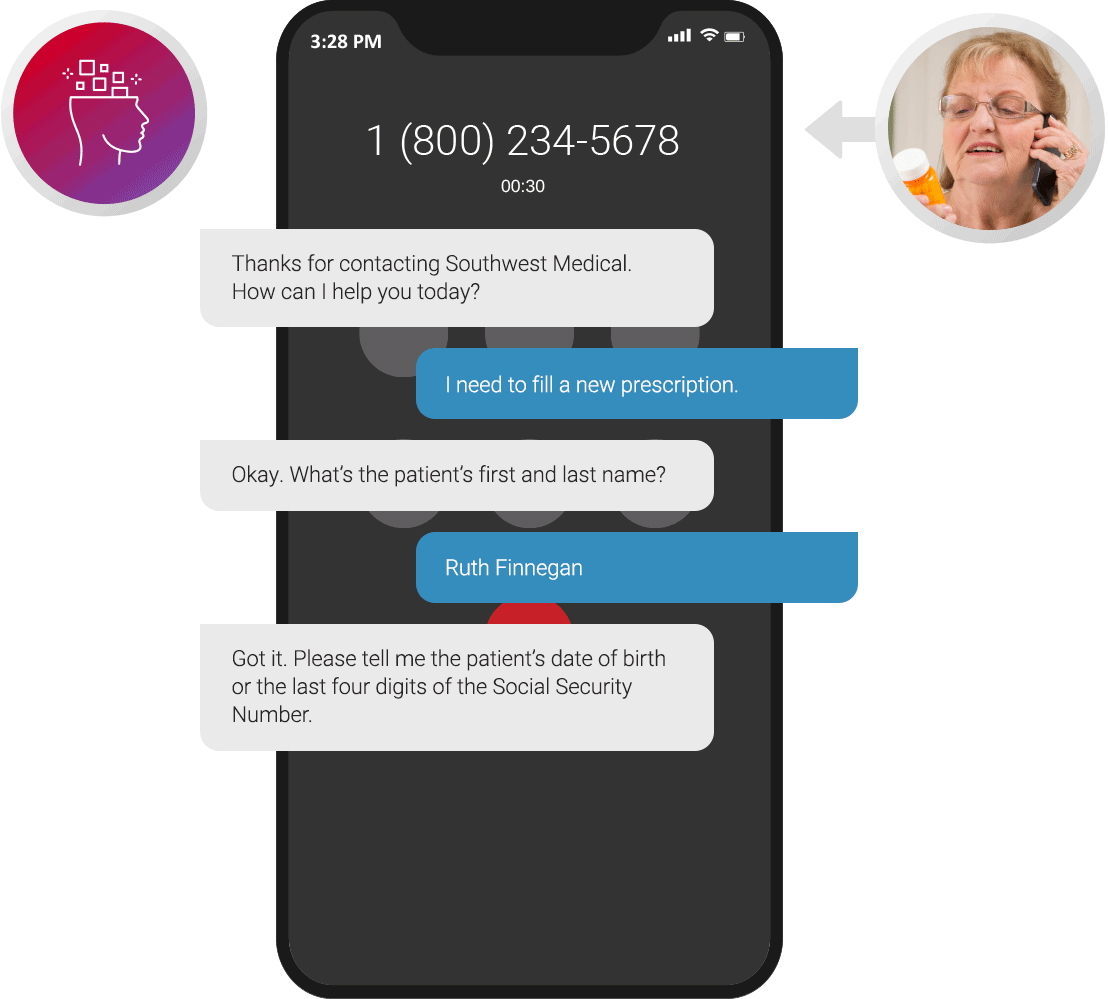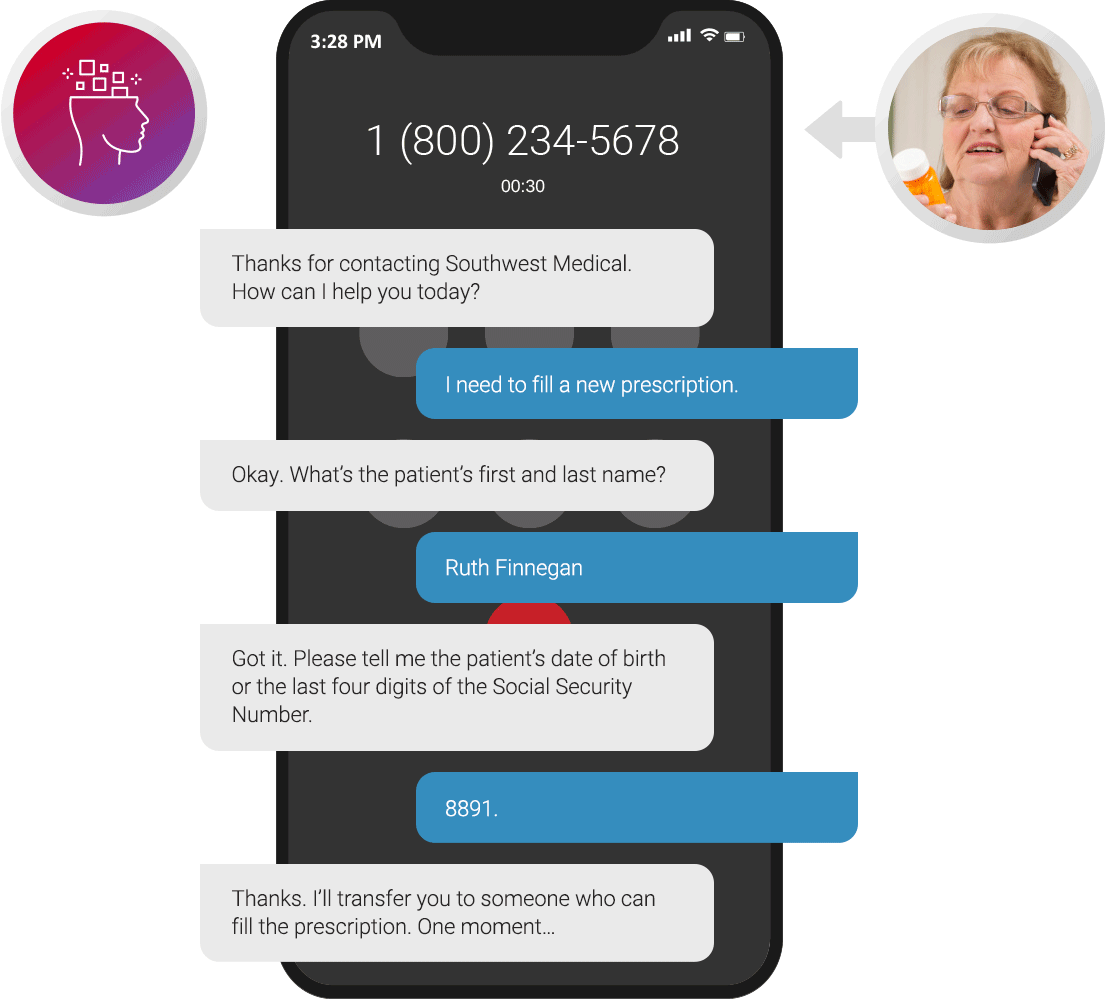
Patient Authentication
Answer every call with a friendly greeting and capture user intent in natural language. Our virtual health agents authenticate patients through HIPAA-compliant protocols and route calls to the appropriate caregiver or department.
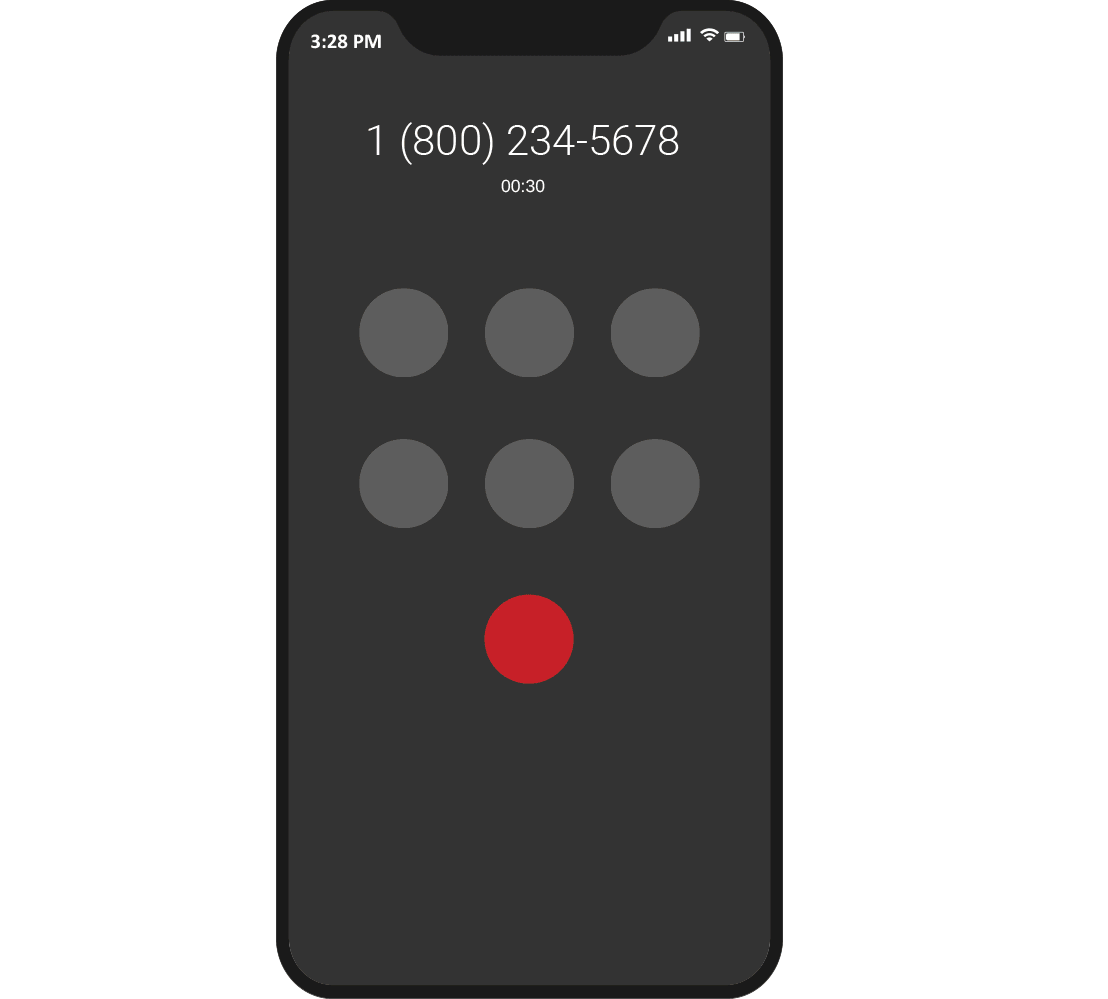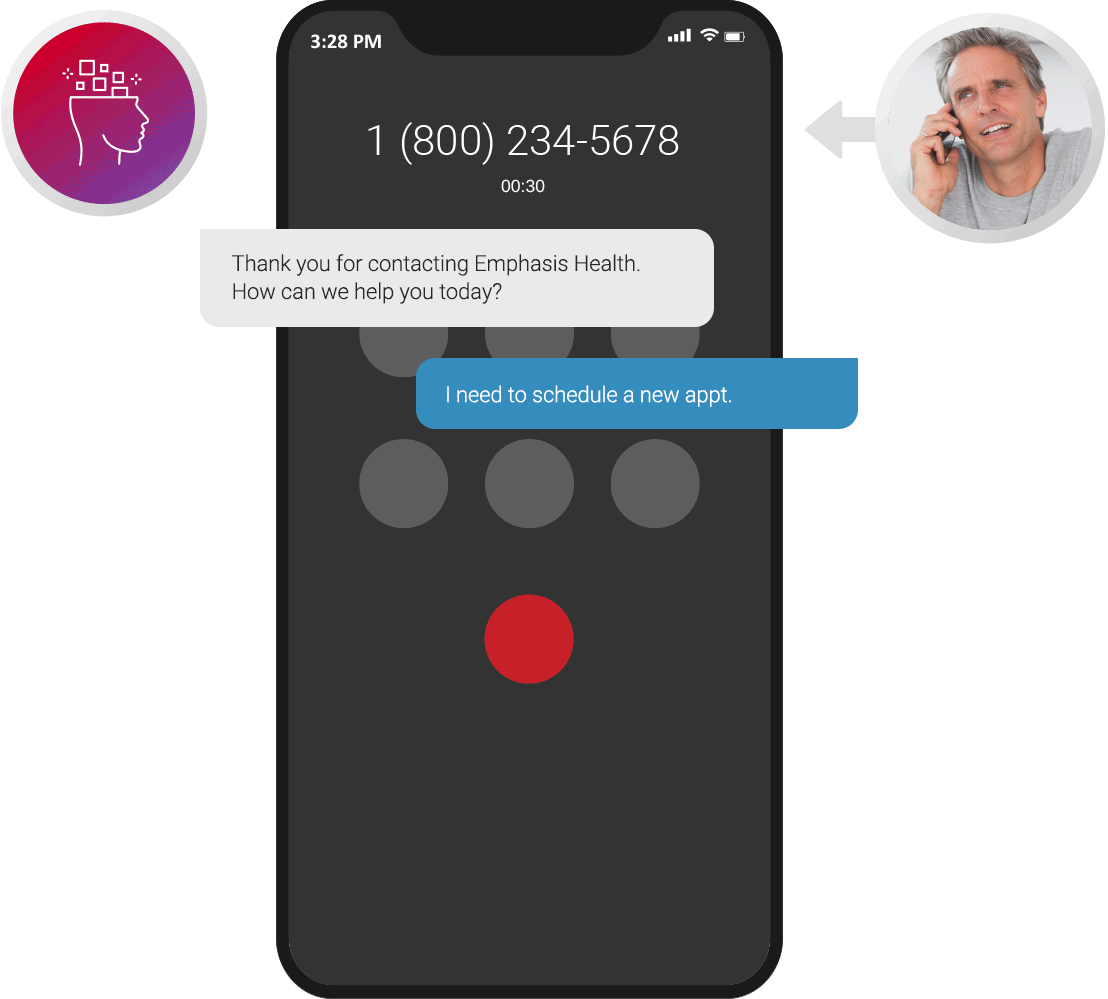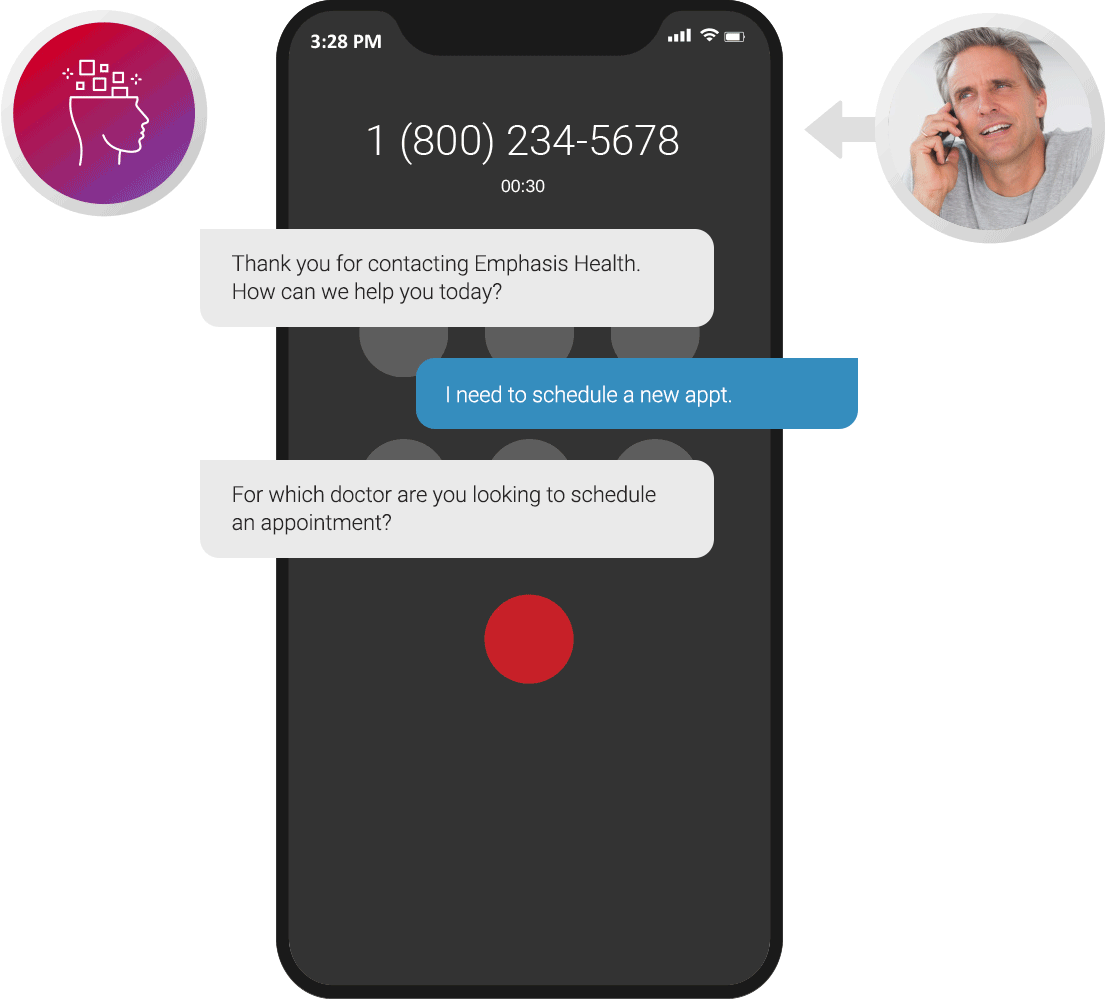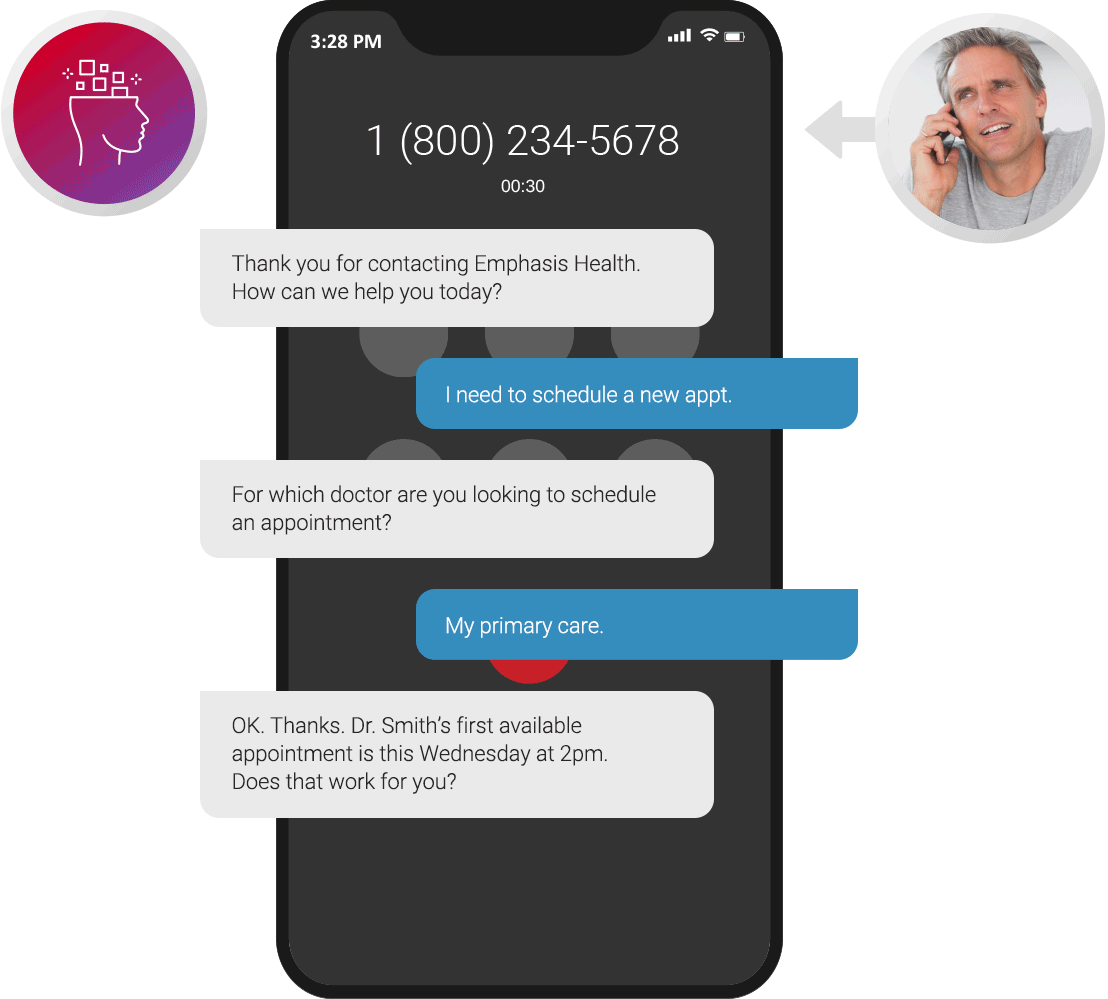
Appointment Scheduling
Nearly all patients schedule doctor appointments over the phone. Our virtual agents excel in scheduling and follow up over outbound voice and text to confirm, modify, get wait-listed or cancel, so you never have a missed appointment again.
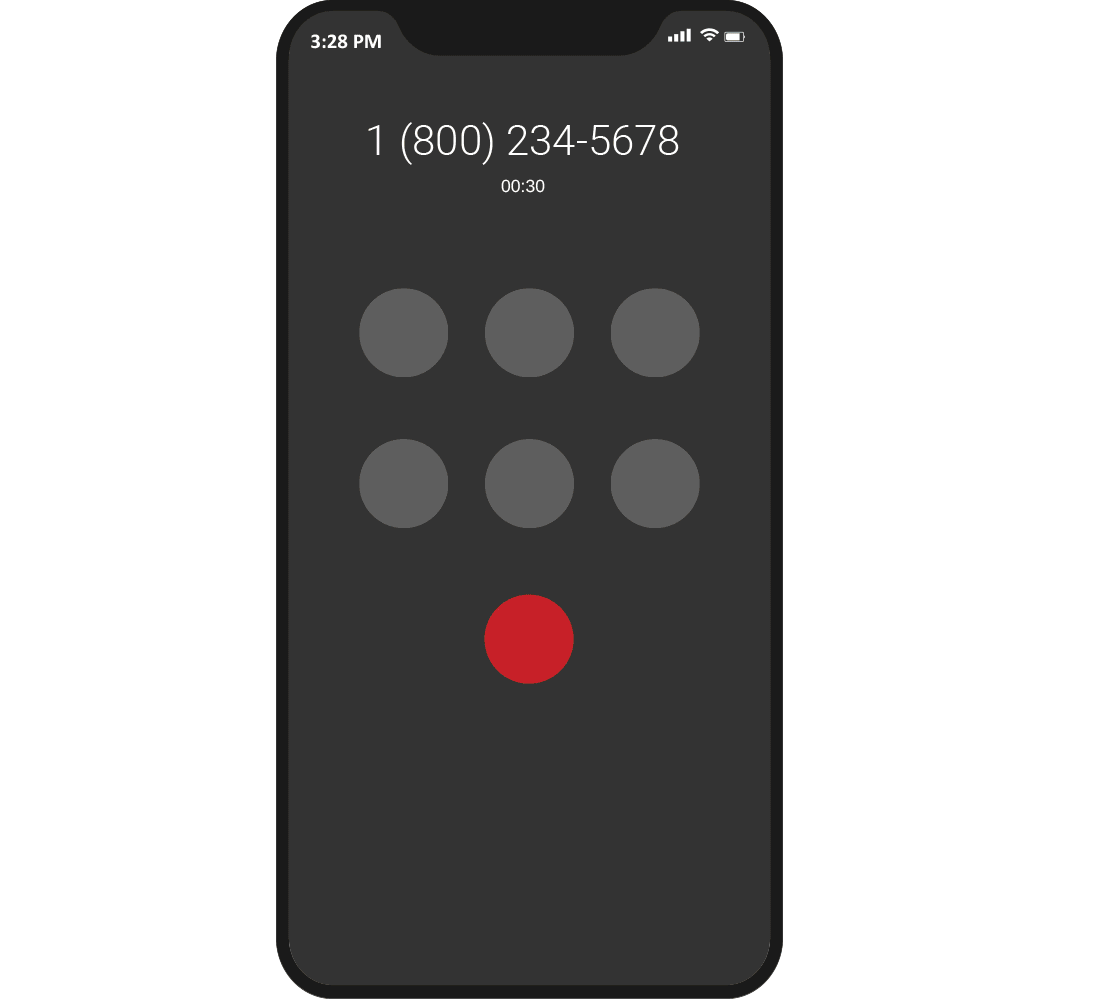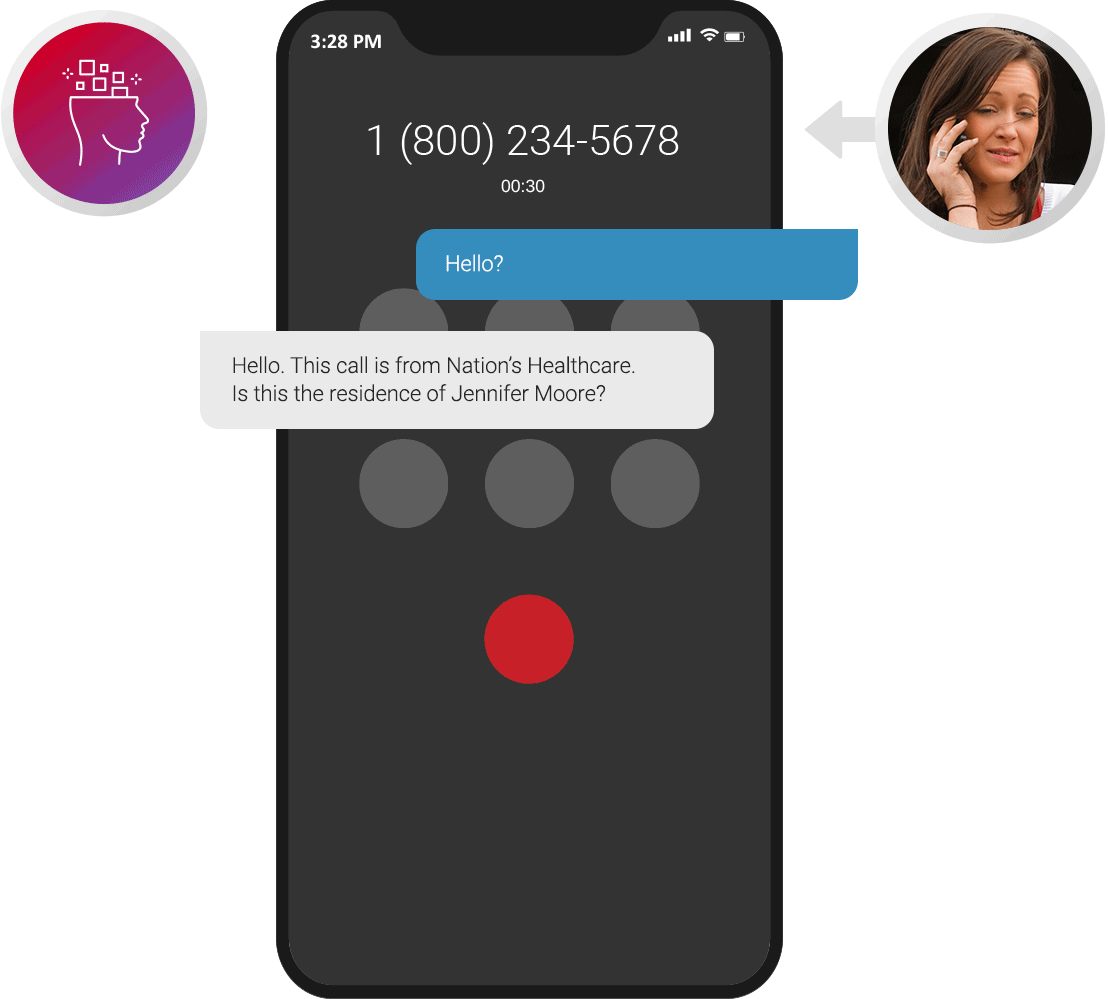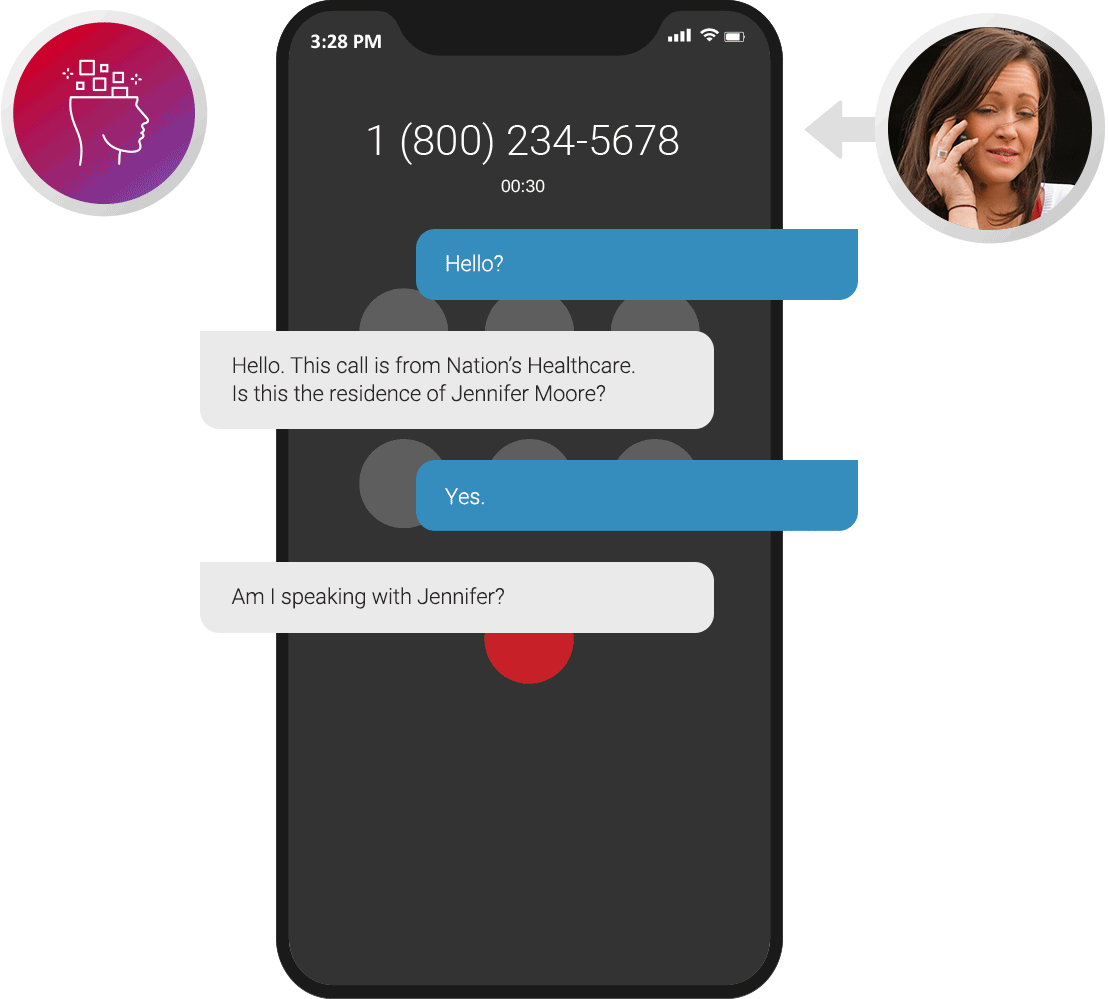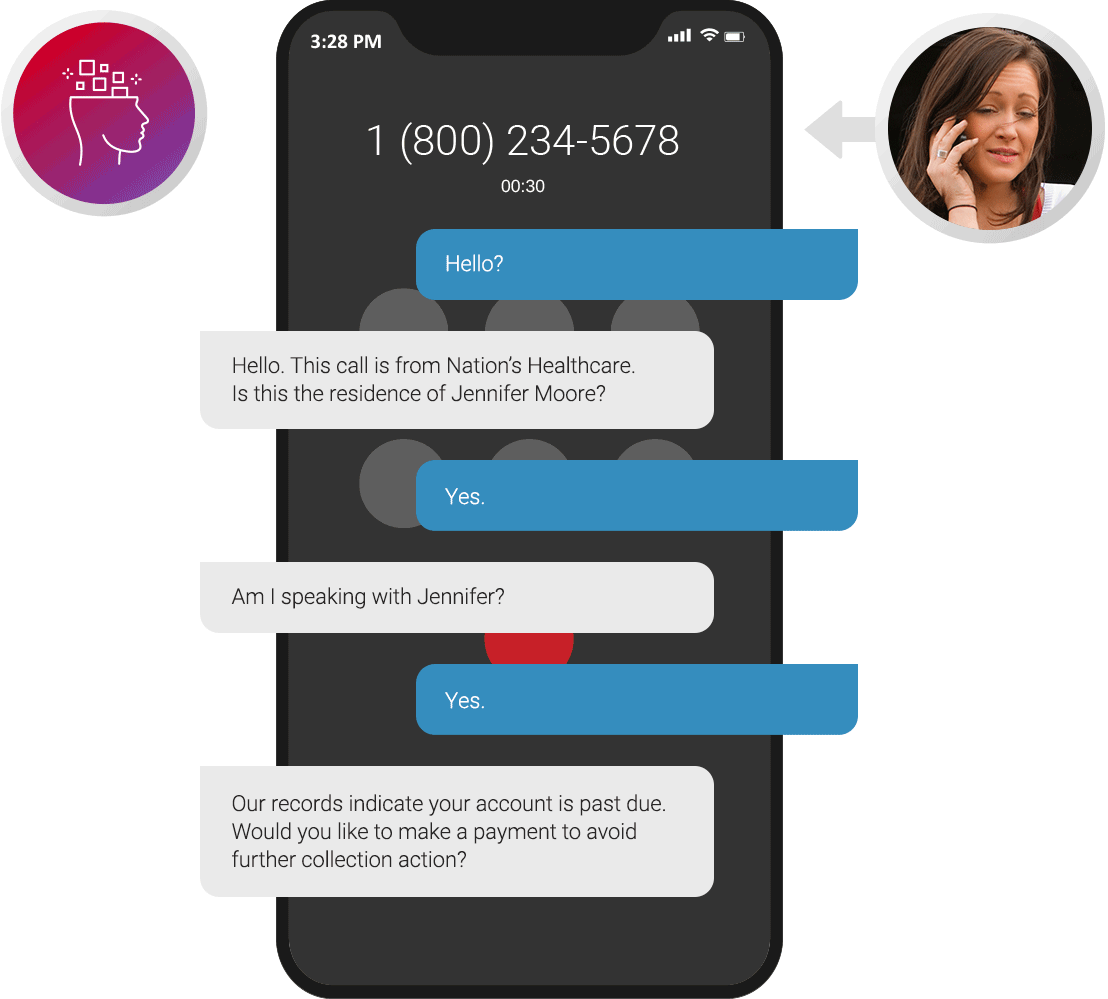
Billing & Collections
Allow patients to get balance notifications and make payments via text, chat, or voice. Resolve outstanding balances faster with inbound/outbound calls to collect payment or arrange payment terms.
Account Management
Facilitate patient access to member services with automated self-service over telephony. Patients can easily change their address on record, update their profile information, and even order medical supplies by simply using their voice.
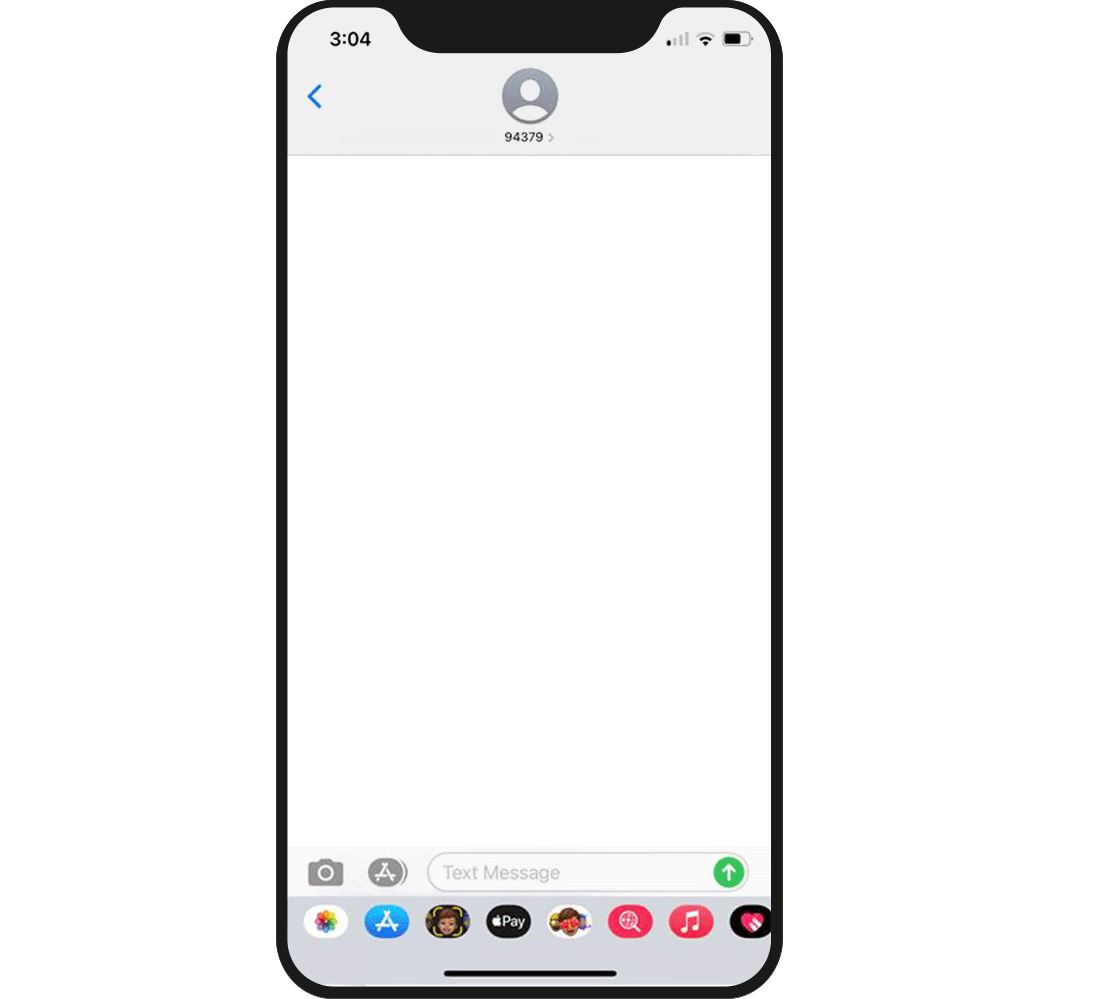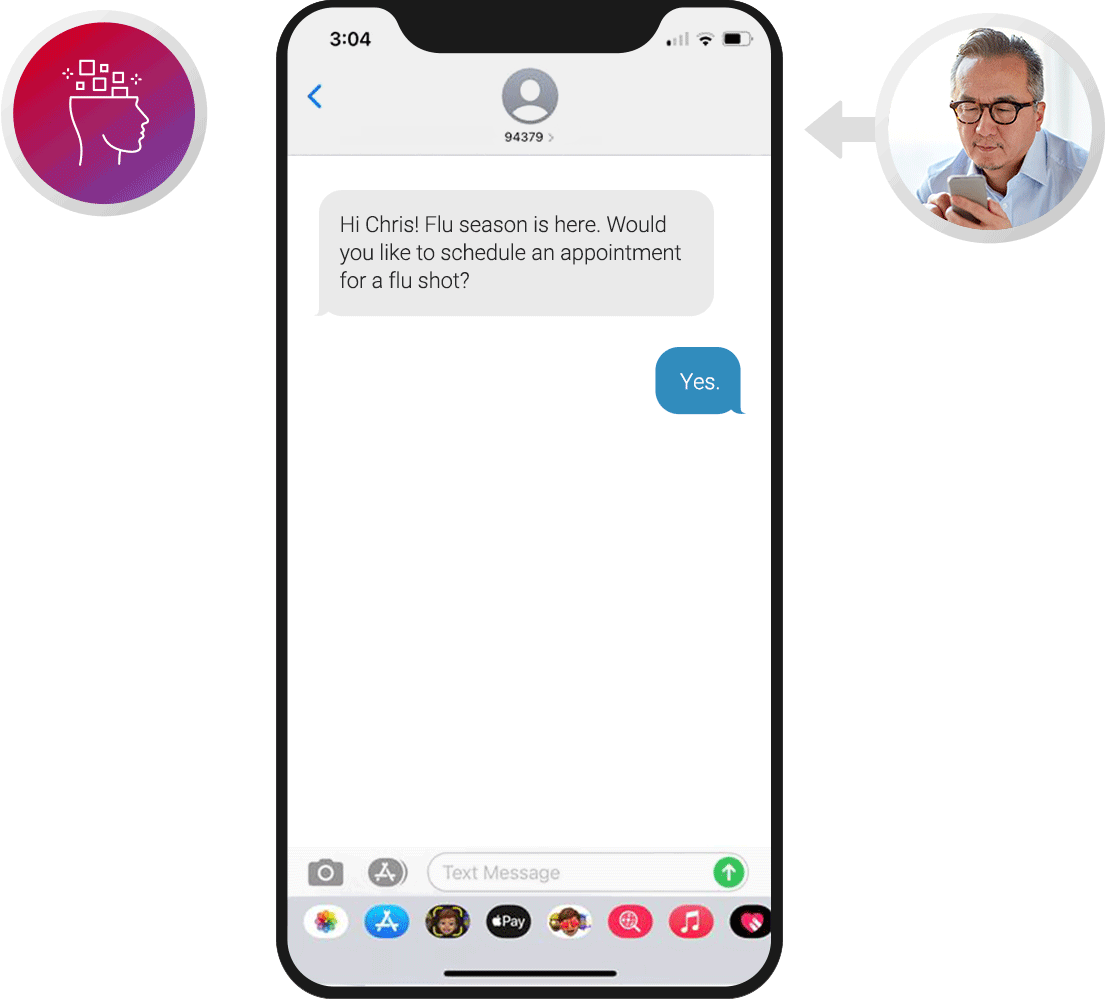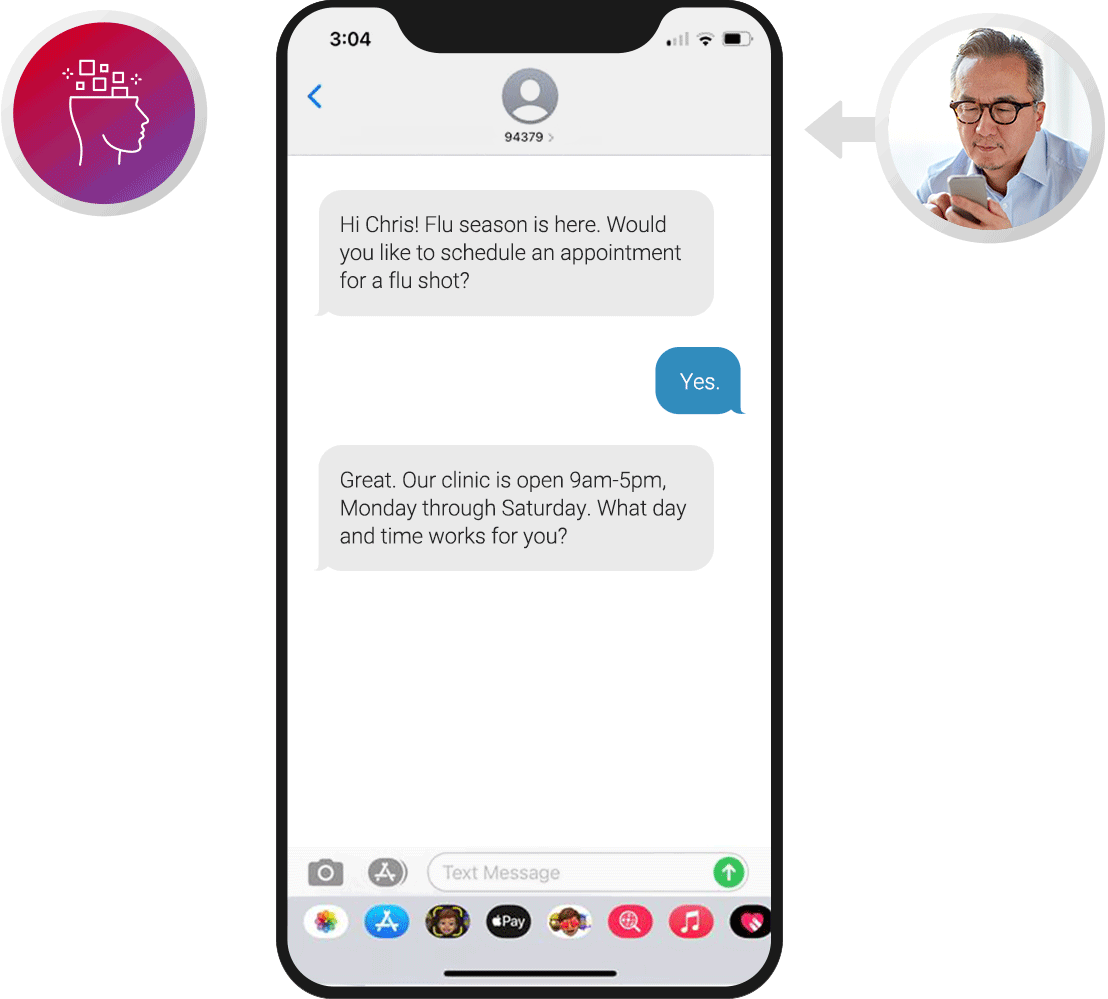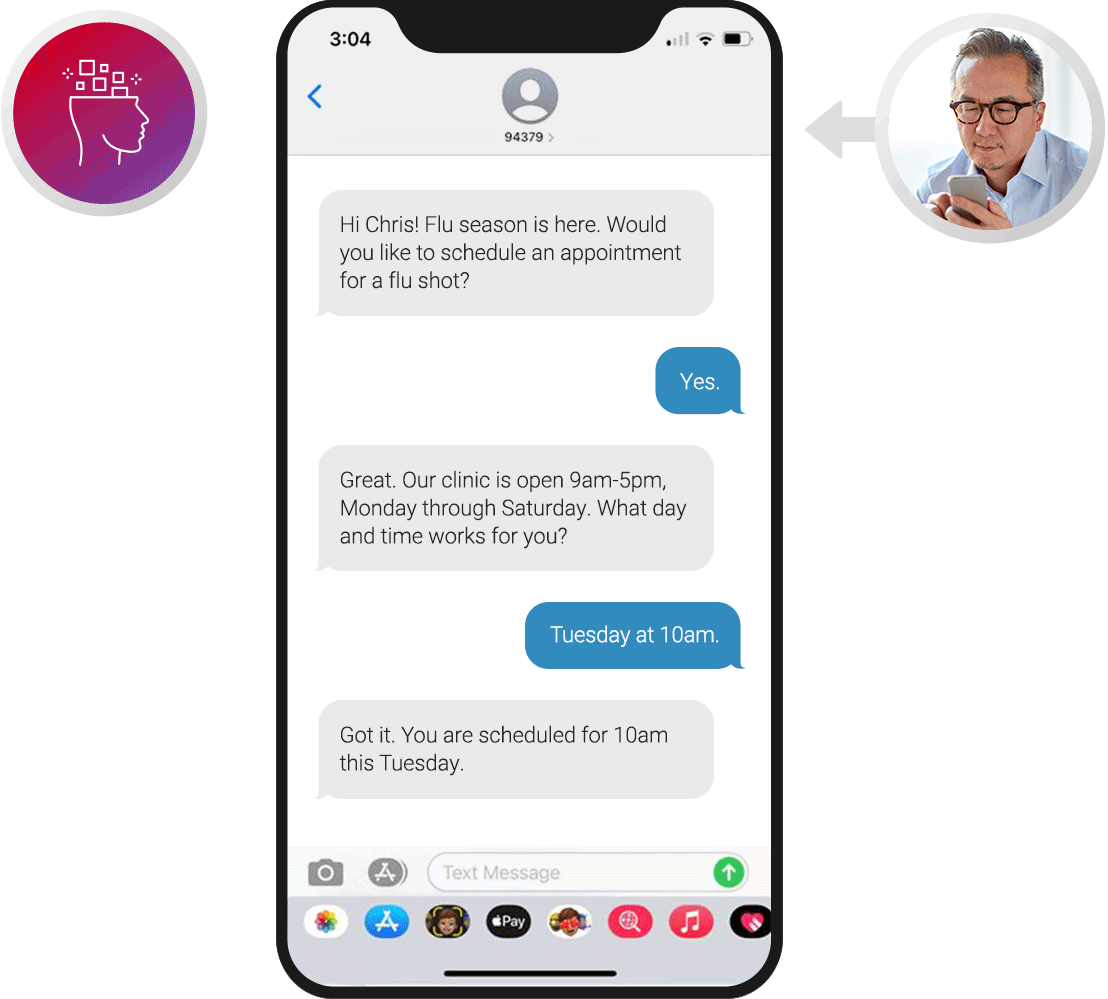
Patient Outreach
Proactively engage patients over voice and digital channels. Remind patients about upcoming visits and provide the option to change or cancel appointments. Offer tips for general wellness, reminders to refill prescriptions, and updates on healthcare services.
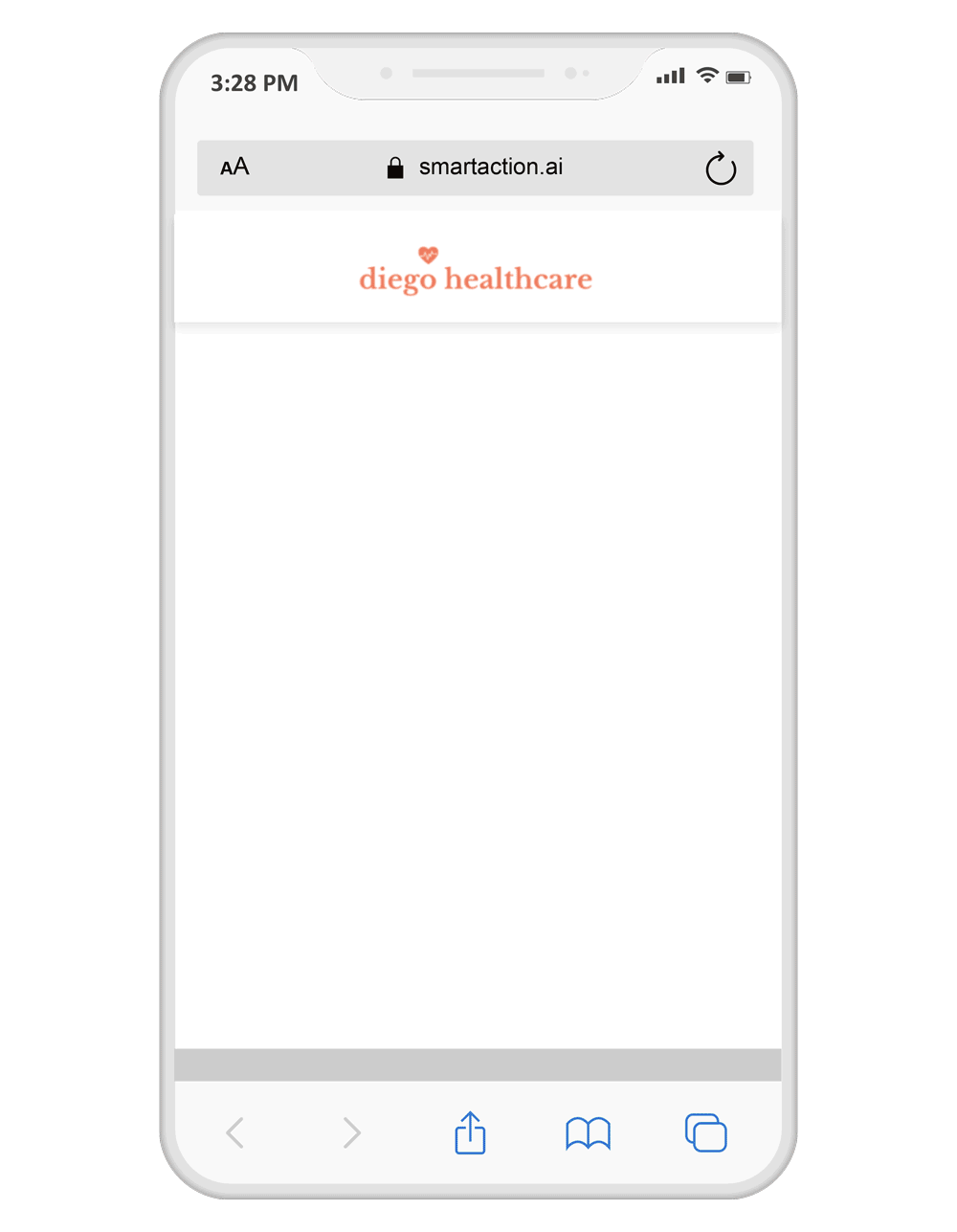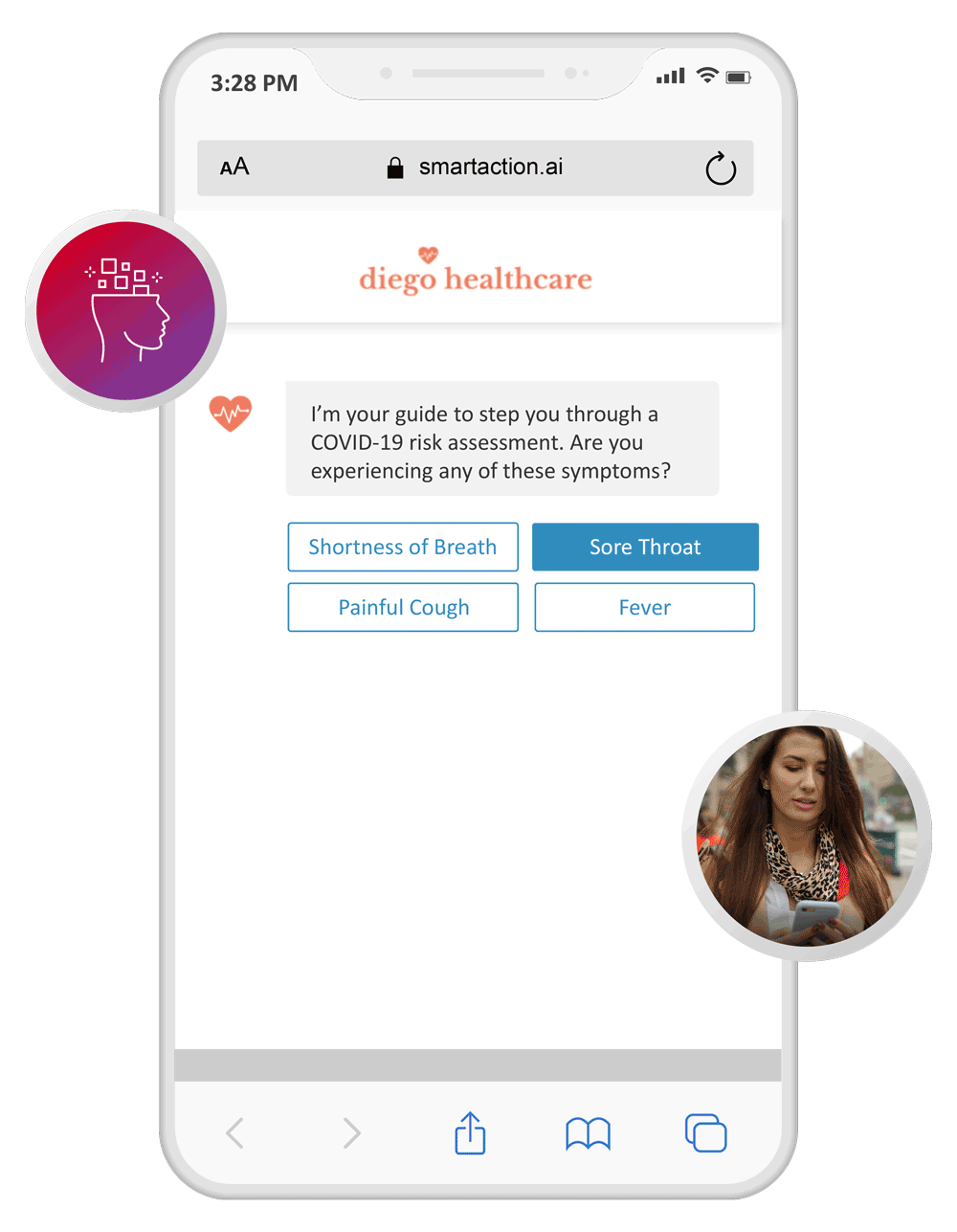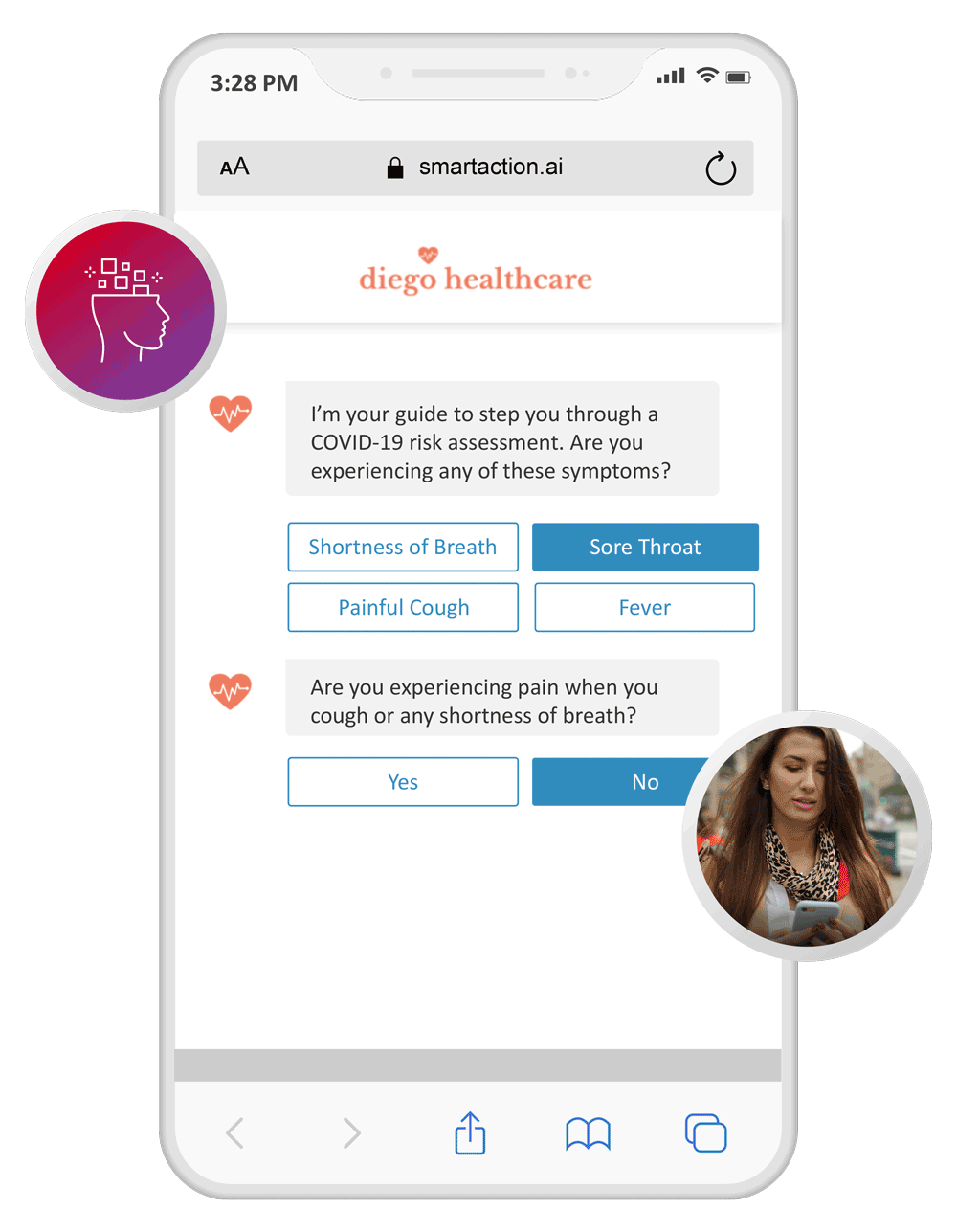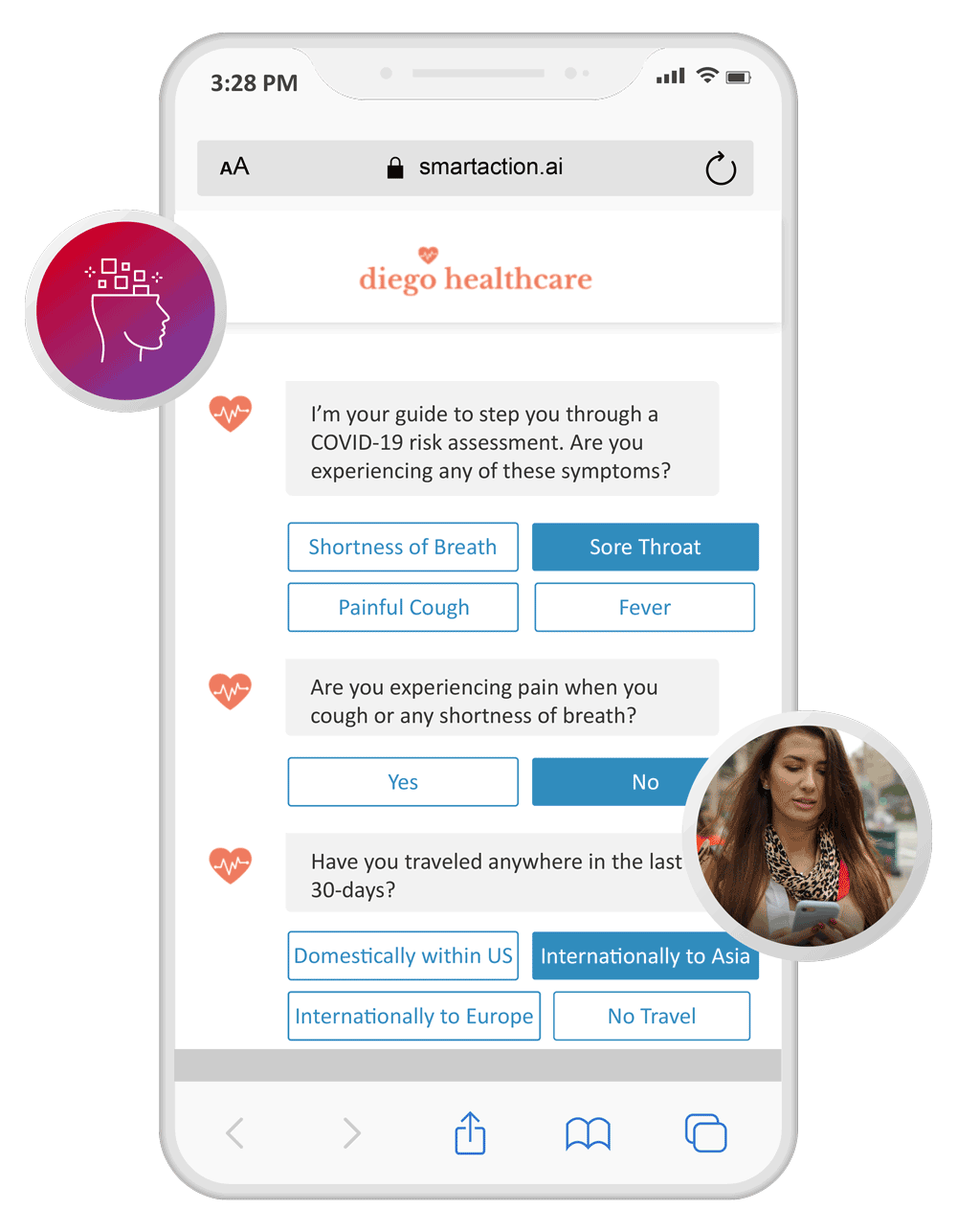
Symptoms Triage
Deflect 100% of COVID-19 related calls to SMS and chat channels, where symptoms can be triaged and an escalation path can be determined. Advise to call 911, go to the emergency department, or receive a callback from a physician.
AI Automation without Patient Frustration
Enhance the Patient Experience
SmartAction’s voice-enabled virtual agents are designed to engage and support patients throughout their healthcare journey.
Improve Patient Access
With SmartAction’s intuitive self-service, patients resolve common healthcare tasks without having to wait for human assistance.
Reduce Missed Appointments
Sending appointment reminders through the communication channels patients use drastically reduces late appointment cancellations and patient no-shows.
Augment Healthcare Workforce
Offloading mundane tasks empower front line staff and call center agents to focus on higher-value work.
96% of online patient complaints center around customer service — not quality of care.
— Vanguard CommunicationsVirtual Health Agents Powered by SmartAction
Conversational Interface
Our virtual health agents help patients resolve issues conversationally — there’s no need to navigate through complex phone menus or install new technology apps.
HIPAA Compliance
SmartAction is fully compliant with HIPAA regulations to safeguard PHI and ensure patient privacy.
EHR integration
SmartAction integrates with all major EHR systems, in addition to your existing contact center infrastructure, to deliver an effortless patient experience.
Omnichannel Experience
Our conversational AI technology engages patients wherever they are and maintains context when switching across voice, chat, and SMS channels.
Data Science Services
We provide custom reporting with data-driven insights to measure call performance, improve the conversational experience, and ascertain ROI.
Dedicated CX Team
Our team of conversational AI experts for voice and chat handle everything for you, from initial design to ongoing operation.
Learn how J&B Medical reduced Patient Effort by 60% with AI-Powered Virtual Agents
Brightree drives $1.88M in Patient Collections


Dr Stephen Shaya
CEO, J&B Medical Supply




